FAQs on Failed Back Surgery Syndrome
 What defines failed back surgery?
What defines failed back surgery?
Nearly 600,000 people undergo back surgery in the United States annually and of that number, many continue to experience symptoms of pain. When a back surgery results in continued symptoms for the patient, the condition is known as failed back surgery (Hildebrandt et al., PubMed, 2010).
Some refer to the condition as failed back surgery syndrome or FBSS, which is related to the continuance of back pain even after surgical procedures have been carried out. There are a variety of reasons why a person may experience pain following surgery, not related to the surgery and healing process, but the continued symptoms that may have occurred prior to the procedure.
What are the causes or reasons for failed back surgery?
Spine surgery is complicated and designed to accomplish four things. These things include:
- The stabilization of a painful joint.
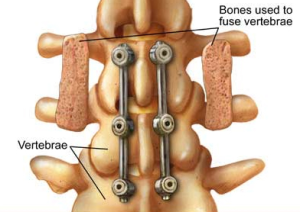
A typical spinal fusion.
- The decompression of a pinched nerve root(s).
- Normal spinal curvature.
- Most of all – PAIN RELIEF!
Back surgery is unfortunately limited in often not being able to completely remove a patient’s debilitating pain and suffering following the procedure. Many people who undergo back surgery are left with pain that remains at 50% or more from the pre-operative status. Or worse, pain remains and prevents them from carrying out their daily activities, including work.
One of the primary causes for failed back surgery is that the original procedure was effective in removing a lesion or herniated disc, but did not eliminate pain (North et al., Johns Hopkins University School of Medicine, 1995). The reason being is that the lesion
was not the actual cause of pain, but rather the changing anatomy of the back and spine or other issues.
Even if a spine surgery is done technically perfectly, if it’s done for the wrong reason, it will not work for pain relief. Another reason for failed back surgery is the surgery was done for the correct reason, but there are multiple pain generators. So residual pain may stay, requiring pain management.
And another reason is if the surgery did not work, meaning the spinal fusion did not take. That would be an indication for a repeat surgery to fix it, rather than simply nonsurgical pain management.
Are there back surgeries that will alleviate pain?
While failed back surgery pain is not predictable there are certain types of back pain that may alleviate symptoms more than others. For example:
- Discectomy – In a discectomy for a lower back herniation (lumbar) that causes leg pain, predictable outcomes are available. The leg pain can be eliminated by the surgery. However, if lower back pain occurs prior to surgery, it may occur after as well. The results are far less successful in removing low back pain than removing overall leg pain. The patient may get rid of sciatica, and then end up with debilitating back pain afterwards. Not really a failed back surgery, just getting rid of half the problem.
- Spinal fusion – This type of surgery may not provide favorable results in terms of pain relief where there is degenerative disc disease in the lower back (lumbar spine). Those patients with degenerative disc disease of the lower back may not receive successful pain relief following surgery (Terzis et al., La Douler Chronique, 2003). Either the pain persists, or is alleviated by 30 to 50% only.
What are the potential causes of failed back surgery other than those listed?
Aside from discectomies and spinal fusions there are several other causes of failed back surgery that may result in pain following the procedure. These include:
- Scar tissue buildup – formation of scar tissue around the root of the nerve. This is often referred to as Post Laminectomy Syndrome.
- Adjacent Segment Degeneration – following surgery the levels adjacent to the original operated levels see additional stresses, break down, and pain increases.
Is there treatment available for failed back surgery syndrome?
Failed back surgery treatment is challenging and covers a wide scope of options. Diagnosing the root cause for pain is important for the treating pain management doctor in order to gain a solid understanding of how best to treat the
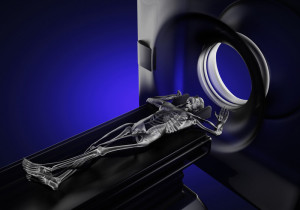
An MRI can help diagnose failed back surgery problems.
problem.
If a fusion or implantation has occurred during the previous surgery, x-rays or a CT scan may be needed to assess the site. The doctor will examine the digital scans to see if the fusion is solid and if the adjacent levels are unstable.
The doctor will also look for scar tissue, especially if the patient reports persistent leg pain. This may necessitate a nerve conduction study.
Medication may be necessary to alleviate some of the painful symptoms, which may include narcotic and non-narcotic pain killers along with neurogenic medications like Lyrica or Neurontin.
Physical therapy and chiropractic treatment along with possibly acupuncture and a TENS Unit may also be ordered to work in combination with other conservative treatments.
Trigger point injections, nerve blocks and steroid injections may also be needed to eliminate pain. If additional surgery is not indicated, as a last resort for treatment of failed back surgery, spinal cord stimulation may be required. This procedure is reserved for the most severe cases of pain where all other forms of treatment for failed back surgery have failed.
Spinal cord stimulator treatment is actually very successful, working well in over 80% of
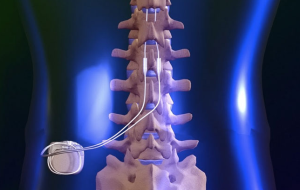
Spinal Cord Stimulator
patients who have the implant placed within 2 years of chronic pain starting.
What is the prognosis and outcome for treatment?
Reasonable expectations are required, as not all treatment may prove to be effective. Patients expecting a 100% recovery from pain may be discouraged when only 75% of the pain is eliminated.
However, your pain management doctor will design the best possible  treatment plan to help eliminate as much pain as possible. A combination of treatment is generally required in order to provide the patient with the best possible outcome. The majority of the time, patients are able to obtain a satisfactory baseline of relief, allowing a return to work and the ability to play with one’s kids and enjoy life again!
treatment plan to help eliminate as much pain as possible. A combination of treatment is generally required in order to provide the patient with the best possible outcome. The majority of the time, patients are able to obtain a satisfactory baseline of relief, allowing a return to work and the ability to play with one’s kids and enjoy life again!


