FAQs of Back Pain – Chronic and Acute
What are the most common types of back pain?
Back pain is among the most common medical conditions, representing the second most common reason for doctor visits and affecting 90% of individuals at some point in life. Most episodes of back pain are resolved within a few weeks, no matter what the treatment received. Up to 10% may become chronic and cause frustrating problems for both patient and the treating physician.
Medically, back pain is separated into two categories: acute pain and chronic pain. Both are common although impact individuals in different ways. Both types of back pain have the ability to cause debilitating problems in the life of the patient, depending on the cause of injury.
What is Chronic Back Pain?
 Chronic back pain is back pain that exists for over three months. It may or may not have an identifiable pain generator. Even the best physicians are not able to identify the exact cause over half of the time. When chronic back pain does have a clear cause, the problem can generally be treated effectively.
Chronic back pain is back pain that exists for over three months. It may or may not have an identifiable pain generator. Even the best physicians are not able to identify the exact cause over half of the time. When chronic back pain does have a clear cause, the problem can generally be treated effectively.
Structural spine conditions, such as spinal stenosis and degenerative disc disease can contribute to chronic back pain that continue unless it is treated appropriately. These conditions can be diagnosed and are due to clear anatomical problems.
The term ‘chronic’ usually refers to pain that lasts more than three to six months and has reached a level that is beyond minimal tissue healing. Chronic back pain may be the result of failed back surgery, fibromyalgia or other problems.
What is Acute Back Pain?
According to research, eight out of ten people are affected by back pain, and most times the pain is acute (Chou, R. et al., Medline Plus, 2012). Acute back pain refers to pain that exists for less than three to six months in duration.
The longer the pain exists, the more susceptible the patient is to chronic back pain. When there is acute pain, rest and ice/heat application can provide relief; also, medications, such as anti-inflammatories may help along with PT and chiropractic treatment.
Can acute back pain become chronic?
The answer to this question is a resounding, yes. Five to ten percent of those with acute back pain will end up with chronic pain. Every case is different and not all patients experience pain the same way. Similarly, not all treatment works the same way. One patient may only require medication and physical therapy to relieve pain for a herniated disc, another patient may end up requiring surgery.
How is Back Pain worked up by doctors?
All types of back pain should receive a comprehensive history and physical exam, checking motor and sensory as well as reflexes. Often times, acute back pain does not require imaging studies.
Chronic back pain sufferers should receive x-rays of the lumbar spine. If there are any “red flags” during the work up, the patient should have blood work and an MRI. A “red flag”  would be:
would be:
- Rest Pain
- Night Sweats/Chills
- Fevers
- Bowel/Bladder issues – this requires an emergency work up.
It is important to distinguish between back pain and pain that radiates into one’s legs. That may indicate either spinal stenosis or a herniated disc, and require an MRI to look for a pinched nerve.
What is the treatment for back pain?
Treatment options vary depending on the cause and nature of the back pain, as well as whether leg pain is associated.
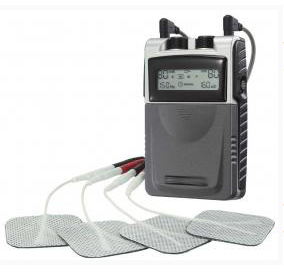
TENS Unit
Typical treatment options for pain that works well is:
- NSAIDs and Tylenol over the counter
- Physical Therapy and Chiropractic Treatment
- Spinal Decompression Therapy
- Acupuncture
- TENS Units
- Trigger Point Injections
- Facet Blocks, Medial Branch Blocks
- Radiofrequency Ablation
- Spinal Cord Stimulator – as a last resort
When leg pain is associated, neuropathic medications such as Lyrica and Neurontin may benefit along with epidural steroid injections.
Less than 5% of all back pain sufferers end up needing surgery. Most of the time, an excellent reduced baseline pain can be achieved with NIPM pain management treatment.



